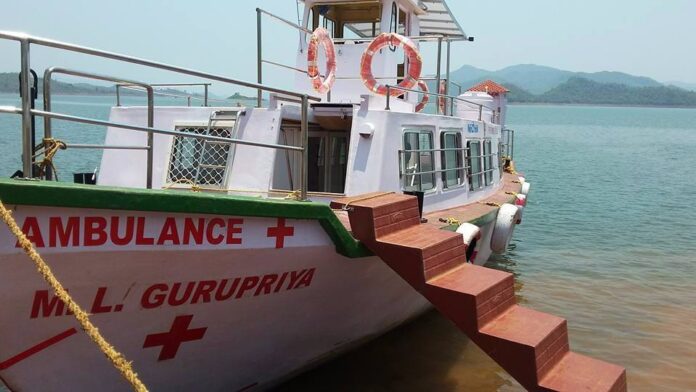
A few months back, the national lockdown to battle the Covid-19 was in its early critical phase and a boat clinic in Assam’s Dhemaji district on the mighty Brahmaputra was on its regular way to a routine camp on one of the thousands of islands or saporis scattered across the riverscape.
By Sanjoy Hazarika
This is a unique geographical phenomenon that many even in the North-east or outside of it know of: nearly three million people or 30 lakh people – or 10% of Assam’s population — live on these islands of which there are not less than 2,500. (Even the author was not aware of these facts till about 25 years ago, and there rests the heart of this story).
The team got an emergency call to head to a small island where a couple in a country boat was bringing a 19-year-old heavily pregnant tribal woman from an island called Mechaki. Their original destination had been the nearest mainland hospital since roads were closed due to the nationwide lockdown. Her husband was far away in Chennai.
The woman had started labour on the boat itself and the family were relieved to catch the sight of the Doctor’s Boat, as it is known there, with professionals aboard. The timing was providential. The young woman medical officer efficiently examined the patient, calmed her parents’ fears and made a quick decision; the delivery had to be then and there on the country boat. The surface was cleaned, necessary hygiene precautions taken, a clean sheet provided, an umbrella gave protection from the sun while a group of women sat around providing privacy.
Exactly 26 minutes later, at 12.26 pm, a healthy three kg baby boy was born much to the delight of the family.
A decade back, the same boat clinic was manned by a different medical unit – many of the young doctors are medical graduates on a rural posting; after a year or two, enriched by the experience, they go back to higher studies and move up in their professional lives.
That earlier time, the boat clinics of Assam were just a few years old. The boat clinic was Shahnaz, named after the late wife of the famous economic editor Swaminathan S Aiyar. Aiyar had been so inspired by the work that he personally donated money for five vessels, which ply in different districts under the names of members of his immediate family.
The SB Shahnaz with its team was returning from days of tiring upstream, treating patients in communities who had long been off the radar and untouched by regular health care.
As the boat moved home, dusk was not far away – it’s not a good idea to be on the river at night especially as few boats, to put it mildly, are equipped to deal with darkness on a vast river – the team noticed a couple waving to them on a small spit of land. They slowed, stopped and anchored. The young couple was desperate because their daughter had acute respiratory distress and was turning blue in the face.
A little more delay and she would have gone. But the doctors had the medicines on the vessel, the SB Shahnaz, they got to work, administered the drugs and the child started breathing easily. The colour returned to her face and her parents signed with relief, smiles returning to their harried faces. The doctors left a supply of medicines for the child and continued their journey.
These are critical choices that the clinics have to take even today, even when overall conditions have significantly improved. These are ‘local’ challenges and immediate decisions that save lives.
The boat clinics have their origins in a winter evening when, during the course of making a documentary film on the Brahmaputra, the filmmaker, Jahnu Barua, and the author were traveling by to Majuli, the great island in the heart of the river.
En route they heard the tragic story of a young woman girl who had died in childbirth on that ferry earlier that day.
The next day, the story became clearer and more tragic: she was a teenager with her first child, a young Mishing tribe woman, who had been carried on a stretcher from the village to the ghat, the ferry landing point which is just a high rise of sand and packed earth. They had missed the ferry that evening and had to stay through the freezing winter night in the embrace of the damp river bank. They took the ferry in the morning but the woman never made it to shore.
Moving by boats, walking across villages and talking to people, as well as a deep dive into the geography and histories of the region helped build an understanding of the unique phenomena of the islands in the Brahmaputra, where people lived, worked and died. There turned out to be some 2,500 villages on almost as many islands on which a tenth of the state’s population lived. This unique challenge needed a unique response, with innovation, clear focus and goals.
The key to making a difference was health access, especially on the islands. People here suffered from a double whammy: geographical and social exclusion. Health services were critical – but the service needed to go topeople not the other way around. The main reason for the young woman’s death in Majuli was that she had not been able to access the service on time. And what better way to get services to people on an island than by boat.
By this time, the author and concerned citizens such the late Dr. Jayanta Madhab had launched the Centre for North East Studies and Policy Research (C-NES) in Guwahati. These looked at issues of good governance and other issues relevant to the region such as connectivity, environment and river transport.
To design the boat clinic idea was not exactly rocket science. There wasn’t a Eureka moment. It needed a combination of common sense, traditional knowledge and people’s wisdom and science, while engaging with respect for the Brahmaputra. Pitched as a Ship of Hope in a Valley of Flood in the World Bank Market Place 2004, competing with 1,500 other entries, the idea won one of the awards – enough to build the first vessel.
The first vessel was built with a combination of inputs from MIT’s design cell, local boat builders and river surveyors and launched in 2005. That vessel, based in Dibrugarh, Upper Assam, the state’s and arguably India’s tea capital, was called Akha (Asha) or Hope. The team had little money, a temporary crew and a couple of researchers. Today, there are 15 boat clinics, of which ninewere built from C-NES’ own resources or funds it had raised. State, national and international and visitors and media are plenty – including the World Bank and UNICEF, diplomats, international media such as the BBC, and ‘national’ and regional media. There is a staff of nearly 200 with teams of doctors, nurses, lab technicians and pharmacists as well as community workers and coordinators who work with district and state administration. Nearly three lakh people are treated every year.
They brave the floods during the monsoons when the river is swollen and high, and storms lash the valley, as well as during the dry season when the river is smaller and shallower with many channels and then walk several kilometers every time they need to set up camp. Villages receive health care at the doorstop with women and children getting priority under national programmes and then come the general checkups. Family planning counseling is conducted regularly with street plays, talks and films. As a result staff report seeing that most difficult of social phenomena – behavioral change with women from the minority community, risking the wrath of husbands and in-laws, coming for contraception, family spacing and a healthier life.
The health workers have been at the frontline of the Covid-19 battle, risking everything to go to the villages during the floods, wearing PPEs and masks. They have given not just counseling, but recorded in-migrants from the lockdown and reported their presence to authorities, ensured they were well taken care of and quarantined. Not less than of C-NES’ 12 frontline workers were infected as a result of outreach work but all have thankfully recovered. In addition, a local philanthropy has supported a programme to supply masks and sanitizers to tens of thousands of villagers in the districts.
The boat clinics were envisaged both a madhyam – a platform for taking not just health care but skills and other services to the island population who are hardy and adaptable. These include sharing knowledge about better nutrition (there is a high incidence of anemia), including introducing the mohingya plant, seeds of which were donated by a philanthropist in Bangalore, and installing solar powered units at Primary Health Care centers, schools and anganwadi centres in Majuli. It has also introduced a solar powered unit that helps the traditional potters of Majuli who never used the potter’s wheel to reduce drudgery and improve health, outputs and incomes.
A question is how did this magical expansion and outreach happen? Of course, the teams are hard working and the public is receptive – although it took a few initial years of foot slogging to win the trust and support of island groups. The success has been dependent on partnership with government. It was clear that to be sustainable, truly effective and reach the last mile, a small NGO could not do it; the biggest stakeholder, the Government, would need to be deeply involved.
That is why credit above all must go to the unstinted backing of one man and his team over the past 12 years in the Government of Assam and the National Health Mission (NHM).
Assam’s Health Minister Himanta Biswa Sarma saw the potential of the programme years back, suggested a partnership, endorsed it and generously offered the funding, networks, medicines, capacity and support of the NHM. He has been the pillar on which this work has run. There have been challenges but the outreach and goodwill that the work has enjoyed is owed to Mr. Sarma’s unstinted backing and his team of knowledgeable and dedicated officers. The latter have been working both at the capital and the district level.
The partnership with the NHM over the past 12 years is worth celebrating – covering all costs of nearly 200 staff including doctors, nurses, pharmacists and lab technicians. Each boat clinic is like a self-contained floating dispensary. The many NHM and Government of Assam initiatives taken together have seen Assam’s measles, mumps and rubella (MMR) fall dramatically from 492 per 100,000 births to 200 in the past of 15 years or so, the best performance to date in the country. It is still the highest but there has been a vast improvement.
This partnership has built the foundation for greater outreach across the state. NHM’s leadership and support has accorded recognition of an idea that germinated on a ferry, after a tragic death, and which has since resulted through a robust public private partnership (PPP) with a non-government organization in bringing health, life and healing to many on the islands of this great river.
The role of the voluntary sector is significant as we have seen. Dr. Poonam Muttreja, the head of the Population Foundation of India, put it well recently: “In India, the spirit of voluntarism, rooted in the tradition of daan, seva, charity and service in all its major religions has been central to the Indian ethos for centuries. But this took on fresh meaning after independence as NGOs forged new ground and helped national priorities to be met and got India going, enabling several government programmes to be implemented more effectively.”
Indeed the Empowered Group 6 aimed at tacking the Covid -19 pandemic under the leadership of the CEO, Niti Ayog, to work with Civil Society Organizations (CSOs), NGOs, development partners and international organizations had earlier this year stressed the significance of this sector, saying it had galvanized “a network of 92,000 CSOs/NGOs … to harness their strengths and resources, expertise in key social sectors-nutrition, health, sanitation, education, and extensive reach in the community… appealing them to assist the State Governments and District Administrations in identifying hotspots and deputing volunteers; delivering essential services to the vulnerable, including the homeless, daily wage workers, migrants, and urban poor families; and in creating awareness about prevention, social distancing, and isolation.”
This article first appeared in www.vifindia.org and it belongs to them. The author is a research associate with VIF.